 Illnesses and disabilities vary in their patterns or
progression over timeand the resulting needs they create. Two important factors affect the needs of the person requiring care:
Illnesses and disabilities vary in their patterns or
progression over timeand the resulting needs they create. Two important factors affect the needs of the person requiring care:
- the rate or speed of the onset of the illness or disability (sudden start vs. slow emergence)
- the predictability of the pattern of recovery or decline
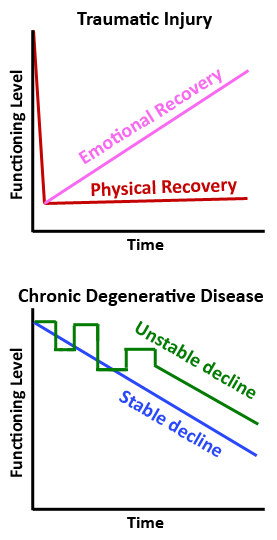
TRAUMATIC INJURY
An acute injury or trauma (e.g., stroke or incident causing traumatic brain injury, spinal cord injury or amputation) has a sudden onset with a significant change in abilities and need for caregiving. Recovery of function is gradual and there is usually uncertainty about the degree of recovery. At the start, theperson requiring care (and the caregiver) often feels overwhelmed by theunplanned change to life.During the recovery process, there are emotional ups and downs.Caregivers must deal with their loved ones’ anxieties,depression and frustrations,along with their physicaland medical needs. The caregiver can do a lot to promote emotional recovery, even when physical recovery is limited.
CHRONIC DEGENERATIVE DISEASE
A chronic degenerative disability or disease (e.g., multiple sclerosis, Alzheimer’s or Parkinson’s disease) has a slow onset. There is a gradual decrease in physical and/or cognitive functioning. There may be periods of improvement, as with some forms of MS, but these are unpredictable in duration and level of functioning. Management of physical symptoms can slow the decline, but good days get fewer as time goes on. Demands on caregivers, both physical and emotional,increase over time.
Finally, congenital disabilities (e.g., cerebral palsy, spina bifida) have a more stable pattern of disability, and caregiving needs are more predictable. Complications associated with aging may arise (as with other types of disabling conditions), but the physical and emotional demands of caregiving are relatively constant.
When a loved one is diagnosed with a chronic disability or experiences a trauma, your life changes forever. You cannot go back to the way it was. Even if your loved one has a full recovery, you become more aware that what you have is both precious and fragile.
 Caregivers typically react to the news
of a loved one’s chronic disabilitywith shock, confusion, fear and a general feeling of being overwhelmed by the situation. Depending on the circumstances, they may also feel anger and a desire to
blame what has happened on someone. These feelings are often shared by the loved one as well. Both go through a process of grief and mourning for what has been lost. During that time,it may be difficult to
take in the information provided by professionals.Whenever possible, get the information in writing so you can make sense of it later at your own speed.
Caregivers typically react to the news
of a loved one’s chronic disabilitywith shock, confusion, fear and a general feeling of being overwhelmed by the situation. Depending on the circumstances, they may also feel anger and a desire to
blame what has happened on someone. These feelings are often shared by the loved one as well. Both go through a process of grief and mourning for what has been lost. During that time,it may be difficult to
take in the information provided by professionals.Whenever possible, get the information in writing so you can make sense of it later at your own speed.
Your relationship with your loved one is bound to change when you add caregiver to your role. Caring for a parent often reverses the relationship you once had and creates uncomfortable feelings for both of you. How will your father feel about you changing his diaper or your mother react when you help her bathe? How will you feel? Caring for a spouse or partner can unbalance your relationship, making household management, finances and decision-making the sole responsibility of one person.
Caregivers have many concerns that often lead to worry and anxiety. What if I can’t keep up the pace as a caregiver? What if I make a wrong decision? What if I can’t advocate well enough to get what we need?What will happen if I am not there when my loved one needs me? What if nothing can stop or control my loved one’s pain and suffering? What if the money runs out? What if I come to resent my loved one’s neediness?
Caregivers often believe that no one else has such negative feelings and that their feelings are wrong or abnormal. None of this is true. However, when fears and concerns are not shared and dealt with, they can become magnified and create greater stress and anxiety. But it doesn’t have to be this way. As the stories in this module reveal, many caregivers have learned that “a problem shared is a problem halved.”