
- The digestive system is complex. A variety of symptoms may appear when it is not working properly.
- Heartburn, constipation and diarrhea are the most common digestive problems that your family members or clients may encounter.
- The symptoms of these common conditions can be managed at home but if the problems continue or get worse, medical care is required.

- Caregivers of older adults deal with a variety of complaints ranging from abdominal pain and swallowing difficulties, through to constipation and diarrhea.
- There are many causes of these problems including diseases, bowel disturbances, infections and medication side effects.
- A digestive problem can be serious in older people. It may cause them to stop eating, which results in weakness and weight loss. These, in turn, can contribute to other problems such as immobility, bedsores and falls.
Common Problems
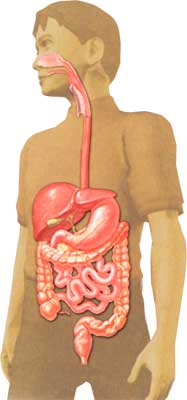 The most common digestive complaints of the elderly are:
The most common digestive complaints of the elderly are:
- Heartburn or reflux occurs when food mixed with stomach acid flows up the esophagus (the tube between the throat and the stomach).
- Constipation involves having fewer than three bowel movements a week, hard stools, and/or straining to pass stool.
- Diarrhea involves having more than three loose stools a day that may be watery or containing mucous.
Heartburn
Heartburn or reflux occurs when food that is mixed with stomach acid flows up the esophagus (the tube between the throat and the stomach). This is the result of a leaky valve between the esophagus and the stomach. Heartburn or reflux can be caused by:
- medications – aspirin, non-steroidal anti-inflammatory medications like Advil or Motrin, osteoporosis medications.
- some foods and drink such as chocolate, fatty foods, tomato sauce, spicy foods, citrus fruits and juices, peppermint, spearmint, caffeinated beverages, coffee and/or alcohol.
- increased abdominal pressure from being overweight, tight fitting clothing or during pregnancy.
- eating while lying down or at a low incline.
- lying down soon after eating a meal or drinking.
- eating and drinking large amounts at once.
Symptoms
Symptoms of heartburn include:
- a burning or gnawing pain in the upper abdomen, which may be worse after eating or lying down (These symptoms of heartburn are similar to that of stomach ulcers. Medical attention is needed if the symptoms become worse or do not get better with treatment.)
- an acid taste in the throat
- a feeling as though something is stuck in your throat
- nighttime coughing
- voice hoarseness
Treatment for Heartburn
 The following may help reduce or prevent heartburn or
reflux:
The following may help reduce or prevent heartburn or
reflux:
- avoid medications or foods that cause heartburn
- avoid lying down after eating, wait 1-2 hours
- eat smaller meals
- lose extra weight
- quit smoking or do not smoke immediately after a meal
- avoid tight-fitting belts or clothing
- raise the head of the bed 10 -15 cm (4” - 6”), it makes it harder for stomach contents to back up in the esophagus
Check with your family member or client’s doctor before giving antacids or any other medication for heartburn or reflux. Antacids may affect the action of other medications they are taking and need. It is important to note that antacids do not prevent heartburn or reflux they neutralize stomach acid masking the problem.
Constipation
- Constipation involves having: fewer than three bowel movements a week, hard stools, and/or straining when passing stool. Constipation can lead to: loss of appetite, blockage of the intestine, hemorrhoids and skin tears in the anus causing great discomfort.
- Constipation is a common problem among older people and can be caused by not drinking enough fluid, medication side effects, consuming a low fibre diet and a lack of exercise or activity.
- Overuse of laxatives can result in a "lazy" bowel, which can make constipation even worse.
- Obtaining advice from your family member or client’s physician is very important when treating constipation.
 Treatment for Constipation
Treatment for Constipation
- Treating constipation should start with a review of medications. Certain medications, such as some blood pressure pills, water pills, and pain medications, can cause constipation. However, often these medications cannot be stopped and other methods are needed to treat the constipation.
- A high fiber diet with increased water/fluid intake (see the Hydration section) can help soften the stool and make it easier to pass. High-fiber foods including: wheat bran, fresh fruits, oatmeal, vegetables, beans/legumes, and dried prunes, apricots and figs may help your family members and clients avoid constipation.
- Increasing exercise activity will also help reduce the risk of constipation.
- Finally, the urge to have a bowel movement should never be ignored.
Types and Use of Laxatives
- Bulk laxatives are useful, but it is important to drink enough water to make the laxative effective. Bulk laxatives such as bran and psyllium (Metamucil, Fiberpur, Prodiem) can be used daily. Start slowly and gradually increase the amount every few days until bowel movements are normal.
- Sugar-type laxatives, like lactulose, keep water in the colon to help the stool move down the colon. They can cause gas and bloating, but are safe to use daily.
- Saline laxatives, such as Milk of Magnesia, also work by keeping the water in the colon.
- Stimulant laxatives, such as Senokot or Dulcolax, should NOT be used frequently. Long-term use can lead to damage to the nerves in the colon, causing it to become "lazy" and making the constipation worse.
Diarrhea
- Diarrhea involves having more than three stools a day and a stool that is loose, watery, or even containing mucous.
- Diarrhea can be short-lived or chronic.
- There are many causes of diarrhea and the treatment depends on the cause.
Cause and Treatment of Diarrhea
- A viral infection or "stomach flu" is a common cause of diarrhea. There is no treatment other than making sure to avoid dehydration.
- Diarrhea can also be caused by a bacterial infection that results after recent use of antibiotics or hospitalization. Medical care is needed, as treatment involves a specific antibiotic.
- Severe constipation can cause diarrhea, when liquid stool from higher up in the intestine seeps past the hard stool. This problem will correct itself once the constipation is treated.
- Many medications can cause diarrhea. Review any medications that were started recently.
- Certain diseases such as diabetes, diverticulitis, irritable bowel syndrome (IBS), Crohn's disease and ulcerative colitis are common causes of chronic diarrhea. Treatment involves managing the specific disease causing the symptoms.
Avoid Over-the-Counter Medications
- Avoid over-the-counter medications for diarrhea (e.g., Imodium or Pepto-Bismol). These medications prevent the body from getting rid of the toxins that are causing the diarrhea in the first place.
- Focus on preventing dehydration by drinking clear fluids such as water, broths and juices. Maintain a bland diet for a few days until the diarrhea subsides.
Wash Hands
Prevent spread of the infection by careful hand washing.
When Medical Attention Is Needed
Medical attention for digestive problems is needed when:
- abdominal pain gets worse or lasts longer than several days
- swallowing is painful
- there is choking or coughing when swallowing
- diarrhea lasts for more than one week
- there is persistent nausea and vomiting
- vomit looks like coffee grounds
- stool is bloody, or black and tar-like
Canadian Digestive Health Foundation
- This website provides a description of the digestive system, including an interactive drawing and information about tests to evaluate your digestive health.
